Bladder and Bowel Problems
Common problems and how to manage them not just with our loved ones but sometimes to ourselves as well.
Information and advice you need to help you love later life.
We’re Age UK and our goal is to enable older people to love later life.
We are passionate about affirming that your later years can be fulfilling years. Whether you’re enjoying your later life or going through tough times, we’re here to help you make the best of your life.
This article about Bladder and Bowel Problems cover the following
- What this guide is about
- How the bladder works
- Types of bladder problems
- How the bowel works
- Types of bowel problems
- Checking for bowel cancer
- Seeking professional help
- What will a health professional need to know?
- Treatments for bladder and bowel problems
- What can I do to help myself?
- Making life easier
- Continence products
- Personal hygiene and comfort
- Dementia and incontinence
- Support from social care and health services
- Claiming benefits
- Bladder or bowel diary
- Useful organizations
What this article is about?
Many people of all ages have a long-term problem with controlling their bladder or bowel, which can have a real impact on their daily lives. This guide looks at different types of bladder and bowel problems and what you can do to help yourself. In many cases, your problem can be cured or managed so it doesn’t interfere with your everyday life.
It’s estimated that 3.4 million people over 65 in the UK experience urinary incontinence and 1 in 10 people may experience bowel incontinence at some time in their life. Many don’t talk about these problems or seek help, often because they don’t think anything can be done. But there are actions you can take to help deal with some of the common problems. Bladder and bowel problems aren’t an inevitable part of getting older. If you’re experiencing them, speak to a health professional.
Throughout this guide, you’ll find suggestions for many organizations that can offer further information and advice about your options. Their contact details can be found in the ‘Useful organizations’ section. Contact details for organizations near you can usually be found in the local phone book. If you have difficulty finding them, your local Age UK should be able to help. As far as possible, the information given in this guide is applicable across the UK.
How the bladder works
The bladder is a muscular, balloon-shaped bag in the lower part of your body that’s supported by pelvic floor muscles. Urine, which is made in the kidneys, passes down the ureters and is stored in the bladder.
When you go to the toilet the bladder contracts, the bladder outlet relaxes, and urine empties out. Your brain controls your bladder, automatically sending messages telling it when to hold on and when to empty.
The female urinary system
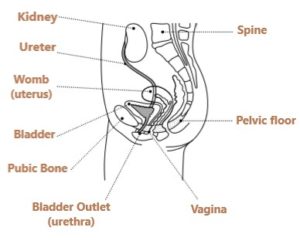
The male urinary system

A normal bladder:
- empties four to seven times each day (every three to four hours) depending on how much liquid you need to get rid of
- can hold up to a pint of urine (between 400ml and 600ml), but usually feels quite full at about half this amount
- may wake you up once at night to pass urine
- tells you when it’s full but gives you time to find a toilet
- empties completely each time you pass urine
- doesn’t leak urine.
Types of bladder problems
There are different types, causes, and symptoms of bladder problems, which can lead to urinary incontinence.
Urinary tract infections (UTIs)
UTIs, such as cystitis, can cause the urgent need to pass urine or a burning sensation when you go to the toilet. They can be painful and uncomfortable, but the symptoms should clear up by themselves after a few days. If they don’t start to improve after a few days, see your GP.
Nocturia
Nocturia is the need to get up during the night to pass urine. If you’re frequently getting up more than twice during the night and it’s disturbing your sleep or making you tired in the daytime, speak to your GP or district nurse.
Stress incontinence
This is when you leak urine as you cough, sneeze, laugh or exercise. Even gentle exercise, such as walking, can cause leakage if you have stress incontinence. It’s more common in women and is caused by a weak bladder outlet and weakness of the pelvic floor muscles that support it.
In women, the bladder outlet is very close to the vagina. The pelvic floor muscles, which support the bladder, urethra, uterus, and rectum, can be stretched and weakened during childbirth. This can lead to a prolapse (when pelvic floor muscles supporting these organs are weakened, causing them to slip). Being overweight can also put a strain on pelvic floor muscles. After the menopause, the body stops producing the hormones that help keep the vagina and bladder outlet healthy.
Men may develop stress incontinence after a prostate operation.
Urgency incontinence
This is where you get a sudden, urgent need to pass urine to the extent that you find it difficult to reach the toilet in time. You may also need to pass urine more often than usual (known as ‘increased frequency’), or this urgency may wake you several times at night.
Urgency incontinence can often be caused by an overactive bladder. Many people find that, as they get older, the bladder gives less warning and needs emptying more often. This is normal until it affects your everyday life or starts to cause incontinence. Then it’s time to seek help.
The reason for an overactive bladder is often unknown. Sometimes it happens following a stroke or other disease of the nervous system when the brain is no longer able to tell the bladder to ‘hold on’ until you get to a toilet.
Urinary retention
This happens when the bladder doesn’t empty completely. Urine builds up and may overflow, often as a frequent, dribbling leakage. You may have difficulty starting to pass urine and feel that your bladder doesn’t empty completely. The stream may be slower than before.
The bladder may not empty completely for a number of reasons:
There may be an obstruction, such as an enlarged prostate gland in men.
If you are severely constipated, your bowel may become over-full and press on your bladder, reducing the amount it can hold or creating a need to pass urine.
Conditions such as multiple sclerosis, a stroke or Parkinson’s disease may make the bladder less efficient at emptying.
Bladder problems in men
In men over 50, bladder problems can be a sign of an underlying prostate problem. If you notice changes to your usual pattern of urination (such as a weaker flow of urine) then visit your GP promptly. If you’re worried about your risk of prostate cancer, speak to your GP about your concerns.
If you notice any blood in your urine, or if you feel pain while passing urine, you should see your GP promptly.
How the bowel works
Food passes from the stomach into the upper part of the bowel. It then passes along the large bowel, where the fluid is absorbed and the remains of undigested food form the basis of a bowel motion (stool or feces). When a bowel motion arrives in the rectum it creates a feeling of fullness. When you go to the toilet, the anal muscle relaxes to allow the bowel motion to pass out through the anus.
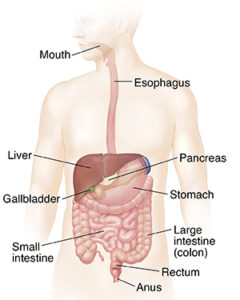
Normal bowel motions:
- are soft and easy to pass
- don’t cause you to strain
- may come several times a day or only once every two to three days (either can be normal).
Types of bowel problems
Many of us experience upset stomachs once in a while or have constipation every now and again. However, if any of these problems happen regularly or are starting to affect your daily life, make an appointment to see your GP.
Constipation
This is a common type of bowel problem and happens when hard bowel motions become difficult to pass.
Constipation may be caused by:
- not eating enough fibre (roughage – found in foods such as wholemeal bread and cereals, fruit and vegetables)
- not drinking enough (you should drink at least six to eight cups of liquid a day)
- not being able to move around much
- some medicines (such as some painkillers)
- not being able to get to a toilet or putting off going (so the feeling that you need to empty your bowel goes away)
- some neurological diseases, such as Parkinson’s Disease
- bowel diseases such as irritable bowel syndrome (IBS).
Diarrhoea
Frequent, urgent, watery bowel motions can cause you to have an accident if you can’t find the toilet in time. Diarrhoea has many causes, including the overuse of laxatives, a bacterial or viral infection, or having IBS or other bowel diseases.
Bowel incontinence
Bowel incontinence is the inability to control bowel movements, leading to accidental leakage of a stool. Some people have this issue every day, whereas others find it only happens occasionally. It’s usually a symptom of an underlying medical condition that affects the bowel (for example, constipation, diarrhoea, multiple sclerosis, stroke).
Bowel incontinence can also be caused by damage to the muscles that control the anus, nerve diseases or muscle weakness (for example, after childbirth). Some women who experience muscle damage in childbirth can develop control problems later in life.
Checking for bowel cancer
Bowel problems can occur in people of all ages and aren’t usually a sign of a serious problem. However, bowel cancer is more common in older people and it’s important to talk to your GP if bowel problems persist for more than four weeks. Bowel cancer symptoms can include blood in stools, change in your bowel habits and lower abdominal pain, bloating or discomfort.
In some parts of England, a one-off test called bowel scope screening is offered to those aged 55 years. For more information, talk to your GP or contact the NHS bowel screening helpline to find out if this is available in your area.
If you notice anything unusual in your bowel habits before you reach this age, or between screenings, don’t ignore it – make an appointment with your GP.
If you’ve reached the age of 60 and haven’t received a kit, or if you’re 75 or over and would like a screening test, call the NHS Bowel Cancer Screening helpline. In Berkshire, call the Berkshire Bowel Cancer Screening Centre helpline 0118 322 7346.
Seeking professional help
If you have a bladder or bowel problem, you may feel uncomfortable telling anybody. But talking about it, especially with a health professional, is the best first step you can take to help yourself. You don’t have to cope alone and there may be a way to manage your problem so it doesn’t interfere with your everyday life.
Bladder and bowel issues should not be considered an inevitable part of getting older. It’s important to talk about them with your GP, the manager of your care home, or the person who is discharging you if you’ve been in hospital, so your continence needs can be assessed.
A health professional who is used to dealing with bladder or bowel problems can assess your symptoms, identify the cause and discuss what treatment or exercises may help tackle your continence problems. Talking things through with friends and family can also be a great support.
Alternatively, ask your GP about your local NHS continence service, where you can have an assessment and discuss your treatment options. Here you will see a specialist nurse, often called a continence adviser. There is a range of other professionals you might be referred to, for example, a physiotherapist or an occupational therapist. To find your local service, ask at your GP practice.
Your GP or continence adviser may suggest a referral to a hospital specialist, who may want to carry out tests to help diagnose your problem.
What will a health professional need to know?
A health professional may ask you some questions to understand how your bladder or bowel is working. We’ve left space for you to make notes here. It’s a good idea to keep a diary of your experiences of bladder or bowel problems so you can give the health professional detailed information. You may also be asked for a urine sample, or your bladder may be tested.
- When did your bladder or bowel problems start?
- How often does leakage happen?
- How much is lost?
- How are you dealing with it?
- How much, what and when are you drinking?
- Can you feel when your bladder or bowel is full?
- Have you noticed any other symptoms, such as pain or discomfort?
- What medications (including over-the-counter and herbal) are you are taking?
Treatments for bladder and bowel problems
Your GP or other health professionals will suggest solutions depending on the type of bladder or bowel problem you’re experiencing. Managing incontinence is an individual thing and sometimes more than one treatment is needed. Here are some common types of available treatment, in addition to self-help described.
Pelvic floor exercises
These exercises may be useful for stress incontinence and urgency incontinence.
A specialist nurse or continence physiotherapist can help you with pelvic floor exercises. Pelvic floor exercises help strengthen the muscles surrounding your bladder or bowel. If you find it difficult to do these, there’s equipment that may help you learn which muscles to use. If you’re unable to contract your pelvic floor muscles, mild electrical stimulation can be used to help exercise and strengthen the muscles.
Bladder or bowel training
Bladder training involves learning techniques to hold urine for longer periods so that you use the toilet less often and gain control of your bladder. These techniques are best for people with urgency incontinence.
Bowel training involves establishing a regular time to have a bowel movement and stimulating your bowels to empty themselves.
Medications
There is medication available for different types of incontinence. Talk to your GP or pharmacist about whether medications might help your problem and what the side effects are. You can find more information on NHS Choice.
While medications are commonly prescribed to treat bowel problems, often these are recommended in addition to diet or lifestyle changes.
Surgery
For some people, surgery may be an option if other treatments haven’t worked. Your GP should talk to you about the benefits and possible risks associated with surgery.
What can I do to help myself?
There are some minor lifestyle changes you could try that may help when you first experience symptoms.
- Drink normally, unless you’re advised otherwise. Aim to drink at least six to eight cups of liquid each day. However, if you’re struggling with nocturia – the need to pass urine more than twice during the night – try restricting how much you drink in the few hours before you go to sleep.
- Tea, coffee or fizzy drinks can make your bladder symptoms worse. Cut down on these drinks or try decaffeinated versions. Drinking too many alcoholic drinks or drinks with artificial sweeteners in them may also cause problems. Pay attention to what you’re drinking and you should soon notice which ones affect you.
- Stop smoking, as coughing can increase pressure on your pelvic floor muscles. Smoking also increases the risk of bladder cancer.
- Keep a healthy weight. Being overweight can weaken your pelvic floor muscles.
- Avoid constipation by eating plenty of fiber-rich foods and making sure you’re drinking plenty of liquid.
- Keep as active and mobile as you can, as this can help keep your bowels healthy. For tips on keeping fit and mobile, see our free guide Healthy living. Contact your local council or Age UK to find out what activities are available in your area.
- Ask your pharmacist or GP whether any medications that you are taking could be disturbing the bladder. For example, water tablets (diuretics) make it fill more often.
Making life easier
You may find that your bladder or bowel problems stem from practical issues, rather than a medical issue. This is sometimes called functional incontinence.
For example, if you have walking difficulties you may find it difficult to reach the toilet in time. Or if your fingers are stiff, it can be tricky to get clothes out of the way quickly enough. You may find it difficult or uncomfortable to get on and off a low toilet. A shortage of public toilets can also lead to problems when you’re out. Incontinence may result from any of these problems if you have an urgent need to pass urine.
If you’re experiencing these sorts of problems, here are some practical measures you can take that may make things easier for you.
Improving access to the toilet
If your incontinence is caused by problems with getting around, grab rails may make it easier to get on and off the toilet. These can be freestanding or wall-mounted. Adding a raised seat to the toilet may make it easier to sit down if you have stiff hips. If you have difficulty getting about, walking aid or stairlift may help you to get to the toilet in time.
Alternatives to the toilet
If you can’t reach the toilet easily, a commode may be useful. These are available in a variety of designs. Many have a lid and look like an ordinary chair when not in use. You can get handheld urinals, for men and women, which can be used in bed or sitting in a chair.
For more advice on special equipment, speak to your district nurse or continence adviser, or contact the Disabled Living Foundation.
Out and about
Try not to let having a bladder or bowel problem stop you from going out. There are practical solutions to problems that might arise. Take spare pads and pants out with you. Scented bags for soiled pants or pads could be useful if you’re worried about the smell.
Toilet queues
The Bladder and Bowel Community offers a free Just Can’t-Wait toilet card, so you don’t have to queue if you’re out and need to use a toilet quickly. You can order one by calling the Bladder and Bowel Community or visiting their website. The card states clearly that the holder has a medical condition that requires the urgent use of a toilet.
You can get a Radar key, which unlocks disabled public toilets that have been fitted with a National Key Scheme (NKS) lock. These toilets are often found in shopping centers, pubs, cafés, and railway stations. Contact Disability Rights UK for more information about Radar keys.
Clothing
Many women find stockings easier to manage than tights, and full skirts easier to get out of the way than tight ones. Men may find loose boxer shorts easier to manage than Y-fronts. Try clothing with elasticated waists, or adapt clothes so that they fasten with Velcro instead of zips and buttons.
Travel
If you’re going on a long journey with family or friends and know you’ll need to use the toilet frequently, let them know beforehand. That way, you can identify potential stopping points and plan for extra stops so you won’t have to worry about accidental leaks.
Continence products
Incontinence doesn’t always respond completely to treatment, but the right products should help manage the problem and let you carry on with normal life.
To qualify for continence products provided by the NHS, you’re likely to need to meet criteria set out by your local NHS. If you’re assessed as eligible for continence products, your district nurse or NHS continence service should arrange the supply free of charge on the NHS. Your health professional will explain what is available in your region.
You can buy many continence products in pharmacies and supermarkets but it’s important to seek professional advice before using them permanently.
Shop around before you buy products, as prices vary. Supermarkets and pharmacies will not charge you VAT on continence products. If you’re buying products online or by mail order, you may need to fill out a VAT exemption form.
There are a variety of pads, pants and other products available. The following are unisex:
- washable products such as reusable pads, which often come as part of a pair of pants
- disposable pads held in place by close-fitting pants, although these tend to be more expensive
- disposable pants, or all-in-one pads with plastic backing and adhesive patches to seal the sides, are generally more suitable for heavy incontinence
- a bed or chair protector in the form of disposable or washable pads.
For men, there’s also a range of appliances that fit over the penis and collect urine into a bag strapped to the leg. A ‘penile sheath’ is the most popular version of this and is available on prescription. Men can also wear pads and pants, or dribble pouches.
If you are having problems with extra laundry, speak to your local social services to see if there’s any help available in your local area.
Personal hygiene and comfort
Skin care
Washing regularly and drying yourself carefully with a soft towel helps to keep skin healthy. If you use a pad, you may want to use a disposable wipe to remove any residue. Change pads regularly. A simple barrier cream, such as zinc and castor oil, applied thinly, will protect your skin. If your skin becomes broken, consult your district nurse or GP immediately as this can lead to a skin infection. A balanced diet and plenty of fluids can also help maintain healthy skin.
If your skin becomes red or sore, make sure that any pad or appliance fits properly and isn’t rubbing. You could also check whether you’ve developed an allergy to something, for example, washing powder or cream, or part of a pad.
Avoiding smell
Fresh urine shouldn’t smell offensive. If it does, there may be an infection. Urine also starts to smell when exposed to the air for long periods. Good-quality pads help absorb some smell. Keep wet clothes or sheets in a bucket with a lid until washed. Mop up spills quickly.
The smell of bowel incontinence is more difficult to hide. Change soiled pads as soon as possible and put them into an airtight container or sealed bag.
Dementia and incontinence
Someone who has dementia may forget to visit the toilet or be unable to communicate their needs. They may not recognize normal triggers that tell us we need to go to the toilet, not remember the way to the toilet, or recognize it when they get there.
In these cases, they might need regular, gentle reminders. If the person you’re caring for forgets where the toilet is, a notice or picture on the door might help. A regular routine can also help, or you may need to learn to recognize signs they need the toilet and discreetly encourage them to go at these times.
If this doesn’t help or you are having difficulties, talk to your GP or district nurse.
Support from social care and NHS
If you are having difficulty at home getting to or using the toilet, speak with social services. They will carry out a needs assessment to find out what help and support you need at home. They can provide support and assistance, such as handrails in the bathroom or a commode.
If problems develop while you’re in a care home, raise them with your GP or district nurse and ask that any long term treatment, including continence products, is added to your care plan.
If you have continence needs or develop problems while in hospital, staff should consider them during your discharge assessment and include them into your discharge plan.
If you’re found eligible for continence products, you shouldn’t have to pay for them. The NHS should arrange for a supply to be delivered to you on a regular basis.
If you’re unhappy with the way your continence needs are met by carers, by staff at your care home or at the hospital, you have the right to complain. Start by having an informal discussion with staff or the managers of the organization providing your care. A relative or friend can make the complaint on your behalf. If you feel your concerns haven’t been addressed, you might want to raise a formal complaint. The organisation must provide you with a copy of its complaints procedure on request.
Claiming benefits
If you have a physical or mental disability and have difficulty getting about, or need supervision or help when carrying out personal care tasks, you might be eligible for Attendance Allowance (AA) or Personal Independence Payment (PIP). These are non-means-tested benefits, so you can claim them regardless of your income or savings.
Having continence issues will not necessarily mean you can get AA or PIP. You may be eligible if you need help with tasks such as getting to and from the toilet, using the toilet, changing your continence pads, or if you need to be reminded to go to the toilet.
Bladder or bowel diary
When preparing for your appointment with a health professional, it can be helpful to keep a bladder or bowel diary for three days. Use the space below to record:
- how much, what and when you’re eating and drinking
- how many times you use the toilet each day and night
- when you go to bed and get up in the morning
- how urgent the need was to pass urine or a bowel motion
- incidences of bladder or bowel leakage and what led to them
- any continence products used
Day 1
Day 2
Day 3

